Plantar fasciitis is a common foot condition that causes pain in the heel and the bottom of the foot. If left untreated, it can become chronic and affect your daily activities.
In this comprehensive guide, we will delve into the various aspects of plantar fasciitis, including its causes, symptoms, diagnosis, and available treatment options.
Whether you are currently experiencing the pain of plantar fasciitis or simply want to learn more about this condition, this guide will provide you with valuable information to help you effectively manage and treat plantar fasciitis.
Understanding Plantar Fasciitis
Plantar fasciitis is a condition that occurs when the plantar fascia, a thick band of tissue that runs across the bottom of your foot and connects your heel bone to your toes, becomes inflamed.
This inflammation can cause irritation and pain, especially with weight-bearing activities like walking or running.
Plantar fasciitis is a common foot problem that affects millions of people worldwide. It can occur in both men and women, and is most commonly seen in individuals between the ages of 40 and 60.
There are several factors that can contribute to the development of plantar fasciitis.
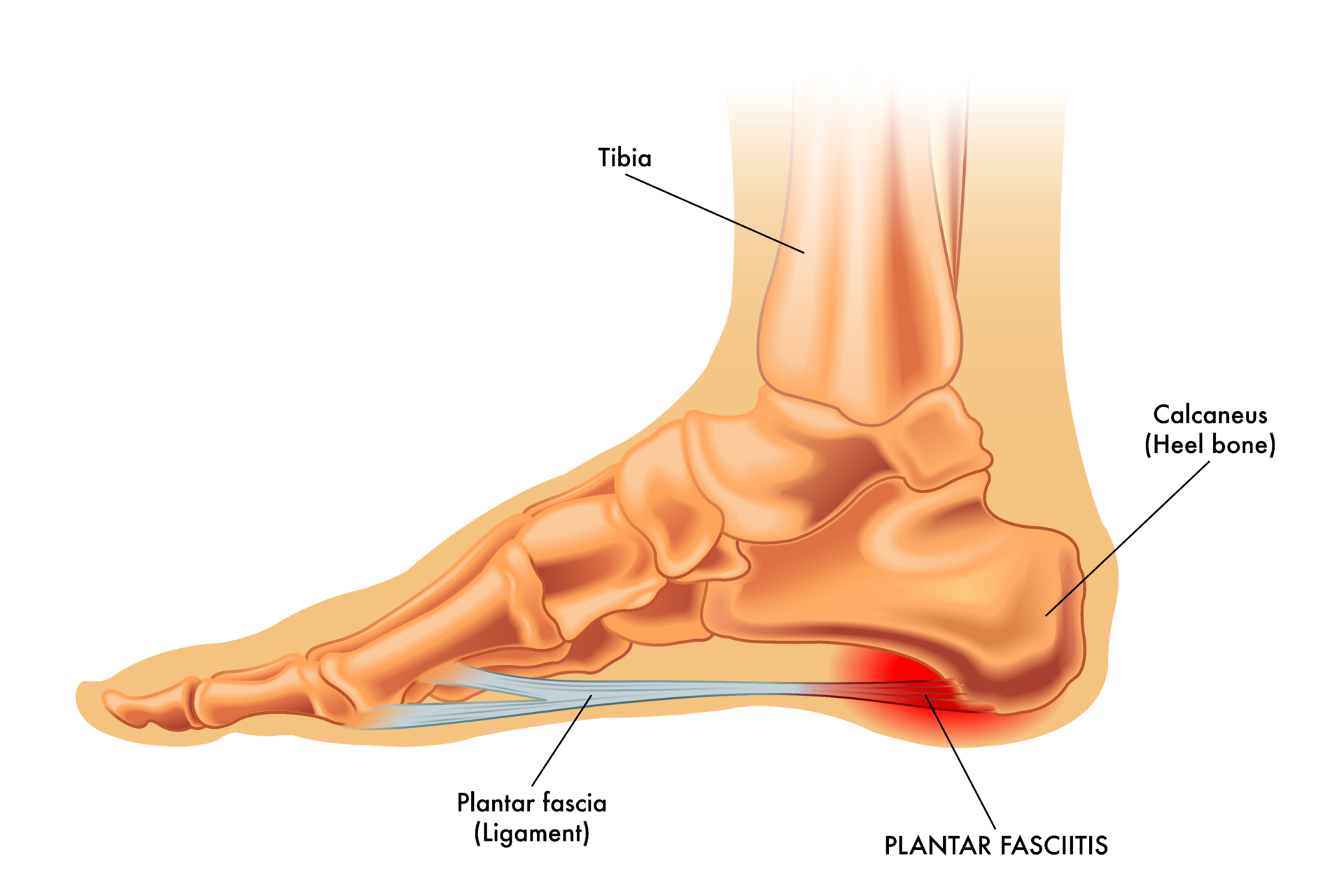
Causes and Risk Factors of Plantar Fasciitis:
Several factors can contribute to the development of plantar fasciitis. Some common causes include:
- Prolonged standing or walking on hard surfaces: Jobs that require long hours of standing or walking on hard surfaces can put excessive strain on the plantar fascia, leading to inflammation and pain.
- Improper footwear: Wearing shoes that lack proper support, stability and cushioning can increase the risk of developing plantar fasciitis.
- Tight calf muscles: Tight calf muscles can put extra stress on the plantar fascia, making it more susceptible to inflammation and injury.
- Obesity or sudden weight gain: Excess body weight can put added pressure on the feet, increasing the risk of developing plantar fasciitis.
- High-impact activities: Activities that involve repetitive impact on the feet, such as running or jumping, can strain the plantar fascia and lead to its inflammation.
- Structural abnormalities of the foot: Certain foot conditions, such as pes planus or “flat feet” and high arch food structures, can alter the mechanics of the foot and increase the risk of plantar fasciitis.
Understanding these causes and risk factors is crucial in preventing and managing plantar fasciitis. By addressing these factors, individuals can reduce their risk of developing the condition or alleviate symptoms if already present.
Symptoms and Diagnosis of Plantar Fasciitis
The primary symptom of plantar fasciitis is heel pain, typically felt as a sharp, stabbing sensation. This can also extend through the middle of the arch along the course of the plantar fascia.
The pain is usually worse in the mornings or after long periods of rest, and tends to improve with movement. In some cases, the pain may radiate along the bottom of the foot towards the toes.
Aside from pain, individuals with plantar fasciitis may also experience stiffness and limited range of motion in the affected foot. It is important to seek proper diagnosis from a healthcare professional if you experience these symptoms, as other conditions can mimic plantar fasciitis.
Diagnosis often involves a physical examination, where the healthcare provider will assess the affected foot for tenderness, swelling, and signs of inflammation.
They may also ask about your medical history and any activities or factors that may have contributed to the development of plantar fasciitis.
In some cases, imaging tests such as X-rays or ultrasounds may be ordered to rule out other possible causes of foot pain, such as stress fractures or tear injuries .
These tests can provide a clearer picture of the foot’s structures and help confirm the diagnosis of plantar fasciitis.
Once diagnosed, treatment for plantar fasciitis typically involves a combination of conservative measures, such as rest, ice, heat, stretch and strengthening exercises, and the use of orthotic devices or supportive footwear.
In more severe cases, additional interventions like physical therapy, corticosteroid injections, or extracorporeal shockwave therapy may be recommended.
It is important to note that plantar fasciitis can be a chronic condition, and it may take several weeks or months for symptoms to fully resolve.
However, with proper management and adherence to treatment recommendations, most individuals can experience significant improvement in their symptoms and return to their regular activities without pain.
Non-Surgical Treatments for Plantar Fasciitis
Home Remedies and Lifestyle Changes
Plantar fasciitis is a common condition that causes pain and discomfort in the heel and bottom of the foot. Fortunately, there are several self-care measures and lifestyle changes that can help alleviate the symptoms and promote healing.
One of the most effective home remedies for plantar fasciitis is ice therapy. Applying ice to the affected area can help reduce inflammation and provide temporary pain relief. It is recommended to apply ice for 15-20 minutes at a time, ideally in the evening when you have “slowed down” for the day. Applying heat throughout the day helps to improve circulation and can aid to reduce pain whilst active.
Rest is also crucial in managing plantar fasciitis. Limiting high-impact activities, such as running or jumping, can give the foot time to heal and prevent further aggravation. It is important to listen to your body and avoid activities that cause pain or discomfort.
In addition to rest, stretching exercises can play a key role in improving flexibility and relieving tension in the plantar fascia.
Simple exercises like calf stretches and toe curls can be done at home and can provide significant relief over time.
Wearing supportive footwear is another important aspect of managing plantar fasciitis. Shoes with good arch support and cushioning can help reduce strain on the plantar fascia and provide additional comfort.
Orthotic inserts can also be used to provide extra support and help correct any biomechanical issues that may be contributing to the condition.
By incorporating these remedies into your daily routine, you can effectively manage plantar fasciitis and prevent further aggravation. It is important to be consistent and patient, as it may take several weeks or even months to experience significant improvement.
Physical Therapy and Exercises
In cases where home remedies and lifestyle changes are not enough to alleviate the symptoms of plantar fasciitis, physical therapy may be recommended. A sports podiatrist can guide you through exercises and stretching techniques specifically targeted at relieving pain and improving foot function.
Physical therapy for plantar fasciitis often includes exercises to strengthen the muscles in the foot and lower leg, as well as stretches to improve flexibility. These exercises can help reduce strain on the plantar fascia and promote healing.
Working with a sports podiatrist can be beneficial as they can provide personalised guidance and ensure that exercises are performed correctly. They can also monitor your progress and make any necessary adjustments to your treatment plan.
Some sports podiatrists also provide Extracorporeal Shock Wave Therapy (ESWT): This non-invasive procedure uses high-energy shock waves to stimulate healing and reduce pain.
Medications for Pain Relief
Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) can be used to manage pain and reduce inflammation associated with plantar fasciitis. These medications, such as ibuprofen or naproxen, can help provide temporary relief from pain and discomfort.
However, it is important to follow the recommended dosage and consult with a healthcare professional before starting any medication regimen. They can provide guidance on the appropriate use of NSAIDs and help determine if they are a suitable option for you.
It is worth noting that while medications can help manage the symptoms of plantar fasciitis, they do not address the underlying cause of the condition. Therefore, it is important to combine medication use with other non-surgical treatments, such as home remedies, lifestyle changes, and physical therapy, for optimal results.
Surgical and Other Medical Treatments
When is Surgery Necessary?
In severe cases of plantar fasciitis that do not respond to conservative treatments, surgery may be recommended. Surgery is usually considered when all other options have been exhausted and the pain significantly affects daily activities.
It is important to have a thorough discussion with your healthcare provider to weigh the risks and benefits of surgery.
Types of Surgery for Plantar Fasciitis
There are several surgical procedures available for the treatment of plantar fasciitis, each targeting different aspects of the condition. Some common surgical options include:
- Plantar Fascia Release: This procedure involves partially cutting or releasing the plantar fascia to relieve tension and allow the tissue to heal properly.
- Tendon Transfer: In some cases, a tendon from another part of the foot may be moved or transferred to support the plantar fascia.
Your healthcare provider will determine the most appropriate surgical option based on the severity of your condition and your individual needs.
Post-Surgery Care and Recovery
Following surgery, proper post-operative care and rehabilitation are essential for a successful recovery. This may include wearing a protective boot, physical therapy, and gradually increasing weight-bearing activities under the guidance of a healthcare professional.
The recovery process can vary depending on the type of surgery performed and the individual’s response to treatment.
Prevention of Plantar Fasciitis
Footwear and Orthotics
Wearing proper footwear that provides adequate support and cushioning is crucial in the prevention of plantar fasciitis. Opt for shoes with arch support, cushioned soles, and a snug fit to minimise stress on the plantar fascia. Additionally, custom orthotics or shoe inserts can help distribute pressure more evenly and reduce the risk of developing foot conditions such as plantar fasciitis.
Regular Exercise and Stretching
Engaging in regular exercise and stretching can help strengthen the muscles in your feet and legs, improving their flexibility and reducing the risk of developing plantar fasciitis. Incorporate exercises that target the plantar fascia, calf muscles, and Achilles tendon into your routine. Remember to start slowly and gradually increase the intensity of your workouts to avoid overexertion.
Maintaining a Healthy Weight
Excess body weight places additional stress on the feet and can increase the risk of developing plantar fasciitis. By maintaining a healthy weight through regular exercise and a balanced diet, you can reduce the load on your feet and minimise the chances of developing foot conditions.
In conclusion, plantar fasciitis is a common foot condition that can cause significant pain and discomfort. However, with proper understanding, early intervention, and appropriate treatment, you can effectively manage and alleviate the symptoms of plantar fasciitis.
Whether you choose non-surgical treatments or opt for surgery, it is important to work closely with a healthcare professional to determine the best course of action for your individual needs. Additionally, incorporating preventive measures such as wearing proper footwear, engaging in regular exercise, and maintaining a healthy weight can go a long way in preventing plantar fasciitis and ensuring overall foot health.
Wrapping Up
Plantar fasciitis is a pain, but you can manage it. If you listen to your body, wear the right shoes, and follow the advice from healthcare pros like Up and Running Podiatry, your trusted Melbourne Podiatrist, you’ll be back in action before you know it!

